Compassionate, Comprehensive Dental Care in Southern CT
Southern Connecticut Dental Group provides award-winning care. Schedule an appointment with one of our CT dentists today to get you a perfect smile!
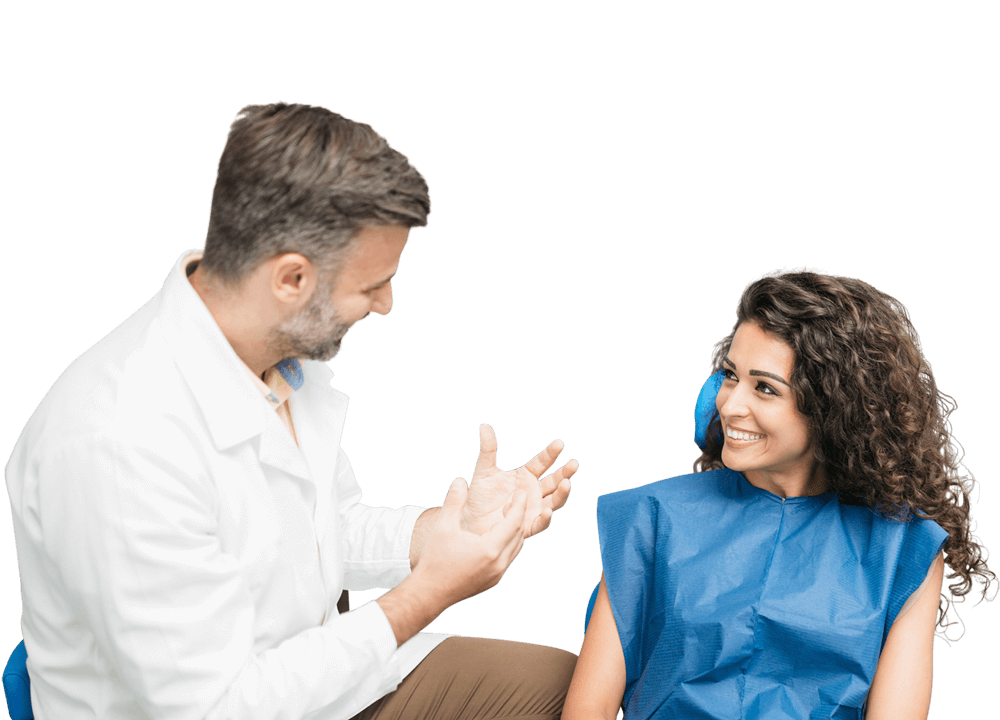
Why Us?
Why Should You Choose Us To Help You Reach Your Dental Health Goals?

Experienced Staff
Each of our dentists is experienced in providing a wide variety of services. They also continuously work on their skills and stay updated with the latest technology through attending regular training.
.svg)
Exceptional Care
Our dentists have a genuine passion for what they do and take pride in helping you achieve your dental goals.
.svg)
Personalized, Comprehensive Focus
We take time to hear your concerns, to discuss your oral health, to provide information and suggestions, and to deliver high-quality dental work when you need it.
CARING, FRIENDLY AND KNOWLEDGABLE TEAM
Meet Our Caring and Compassionate Team of Dentists.
Our clinical teams are comprised of general dentists and dental specialists in Connecticut, making our two locations general, cosmetic, and multi-specialty dental offices. We deliver the highest level of clinical care. Using state-of-the-art equipment and technology, our general and specialty dentists provide comprehensive care for the whole family.
Stephen C. DiBenedetto, DDS, FAGD
Dental Director, Southbury
Lindsay Gadzik, DDS
General Dentist
Stacey Zirilli, DMD
Dental Director, Southbury
Virginia Graicerstein, DDS
Dental Director, Ansonia
Anushka Prakash, DDS
General Dentist
James Pucci, DDS
Periodontist
Thomas DeRienzo, DMD
General Dentist
Meghan Graham, DMD
Orthodontist
What we do
Our Comprehensive
Dental Services

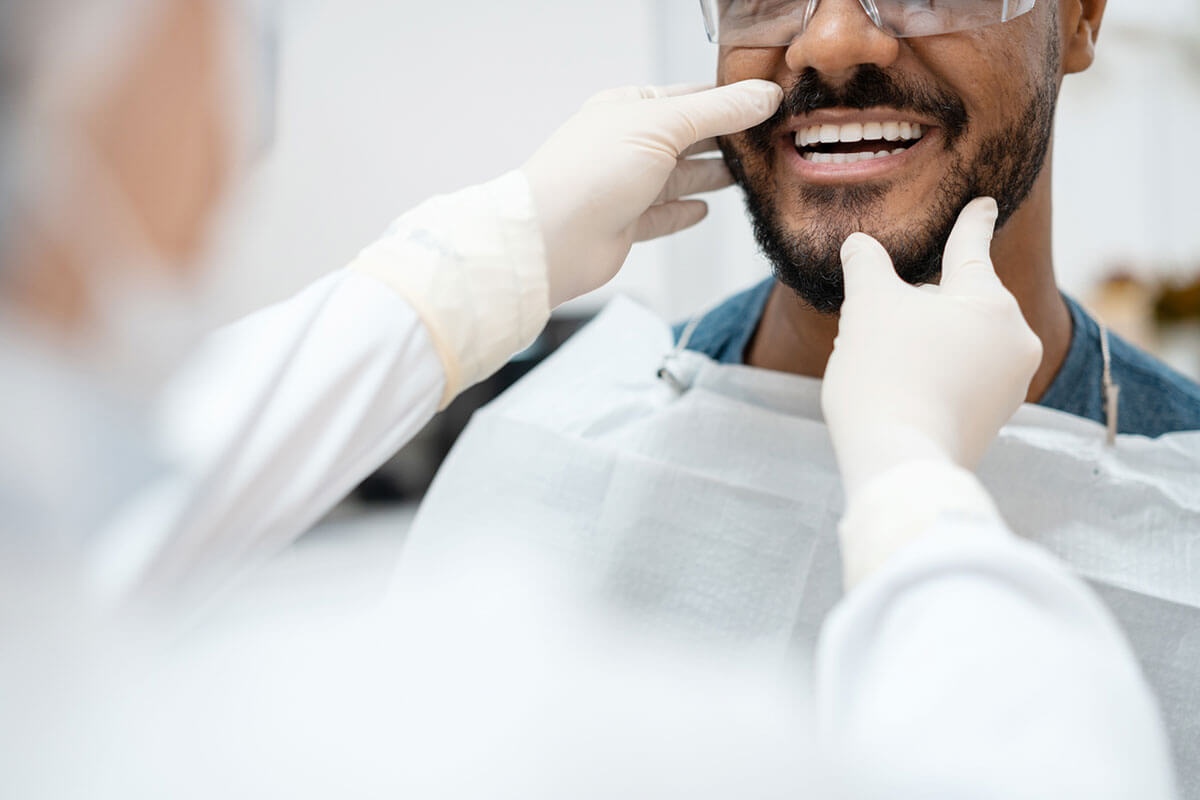

SAVE AT Southern Connecticut Dental GROUP
Dental Offers
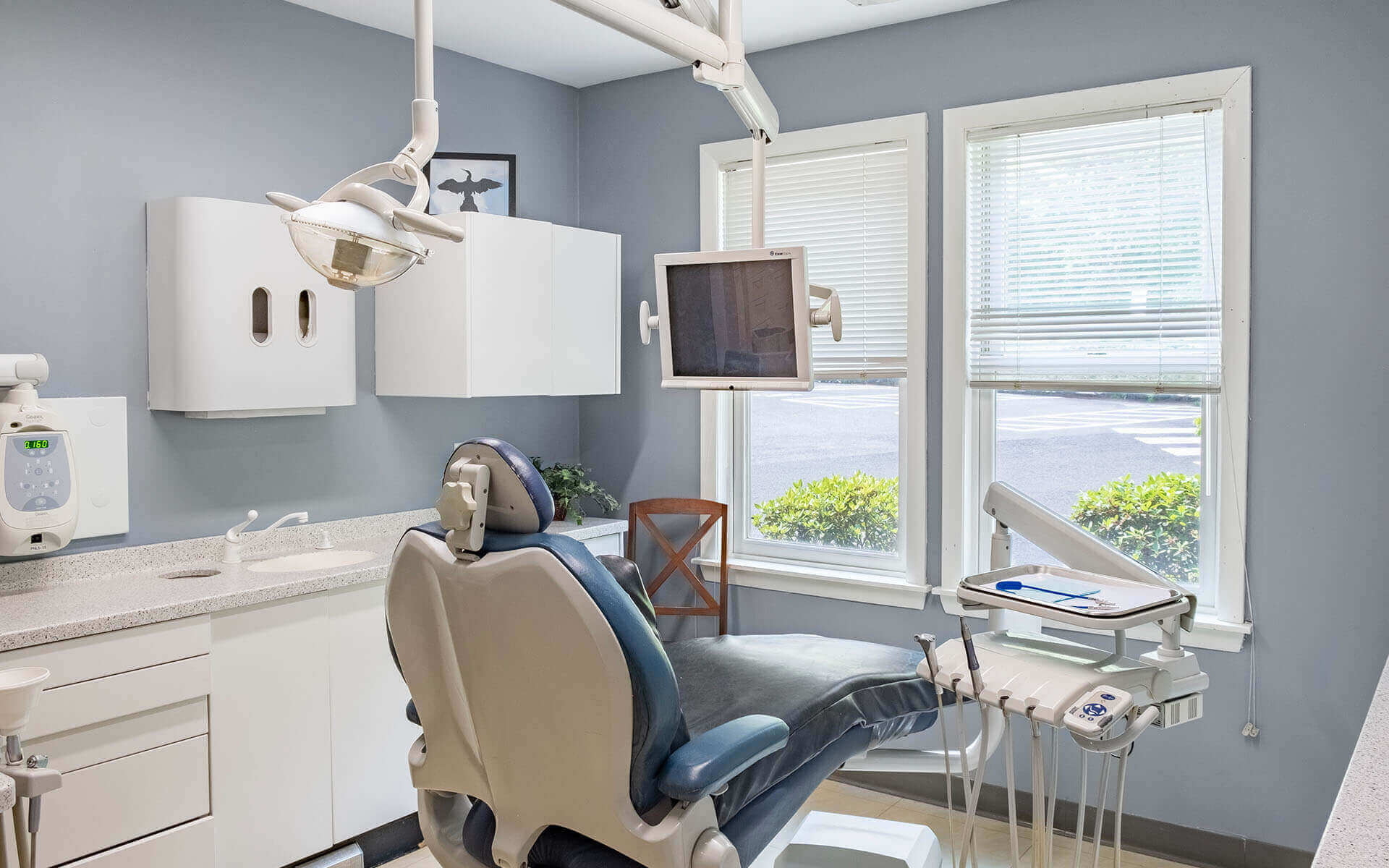
About US
Southern Connecticut Dental Group is a healthcare leader in Connecticut.
Southern Connecticut Dental Group offers high-tech dentistry with a gentle touch. Our offices provide comprehensive dental care services to the CT area. From dental fillings to emergency dental care, our team will work with you to listen to your needs and concerns. We know how important having a healthy smile is, so we take a proactive approach to creating the most appropriate treatment plan for you.
Insurances we honor
We Are In-Network Preferred Providers for All Major Dental Insurance Companies
Not sure if we work with yours? We’re happy to check!